When choosing health insurance for your company, there are many decisions to make. One of the first may be what type of plan to choose.
If you’re looking for health insurance, you’ve probably come across the acronyms HMO, PPO, POS, and EPO. That’s a lot of letters in one place. Here’s what each stands for:
HMO: Health Maintenance Organization
PPO: Preferred Provider Organization
POS: Point of Service
EPO: Exclusive Provider Organization
Understanding the differences between these options is an important first step to determining which kind of plan is right for your company and employees.
Understanding HMO, PPO, POS, and EPO Insurance
To begin, here’s a general overview of the differences between these four plans. We’ll break down these differences in more detail later in the post.
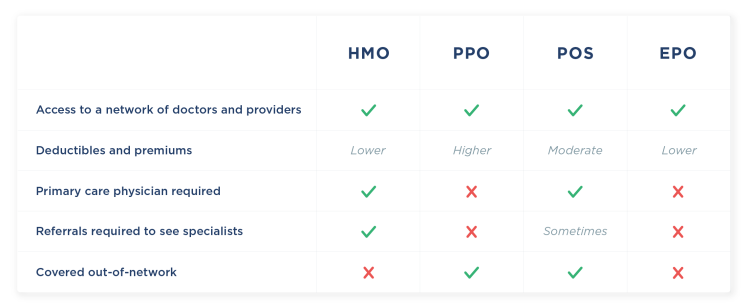
The best way to understand the differences between HMO, PPO, POS, and EPO is to break down how they are structured.
HMO: Health Maintenance Organizations
HMOs begin by establishing a local network of doctors, hospitals, and other providers. The providers agree to accept payment at lower rates for the services they provide to plan members, which sets costs and keeps them in check. HMO plans typically require patients to have referrals from a primary care physician, and won’t cover out-of-network care.
PPO: Preferred Provider Organizations
PPOs also offer access to a network of doctors and providers who accept payment at a certain rate for members. However, unlike an HMO, a PPO allows patients to access treatment from providers outside of the network. In other words, members of a PPO can see any doctor they want or visit any hospital, although providers outside of the network will tend to cost more. Patients are also not required to choose a single primary care physician, and do not need a referral to see specialists.
POS: Point of Service
POS provides in-network care like HMO, but also allows patients to receive out-of-network care under certain circumstances. POS plans are typically gated, meaning a member must choose a primary care physician who is the “point of service.” However, this is not always the case.
As with Preferred Provider Organizations or any other plans covering both in- and out-of-network services, if you choose to access healthcare services from providers outside of your network, you'll have higher out-of-pocket costs, and not all services may be covered.
While similar to HMO, POS plans provide more geographic flexibility (as well as out-of-network benefits).
EPO: Exclusive Provider Organizations
EPO also provides access to a network of providers. Like HMOs, these plans do not pay for out-of-network care (except in some emergency circumstances). Unlike HMOs, EPOs usually do not require patients to select a primary care physician and do not require referrals to see specialists.
Cost of HMO, PPO, POS, and EPO Insurance
Cost is a major factor in choosing between plans. While every plan differs, in general, the more flexibility a plan offers — e.g., covering some percentage of out-of-network care or allowing patients to see a specialist without a referral — the more it will cost in terms of premiums and cost-sharing (e.g., deductibles, coinsurance, and copayments). The less flexibility, the less expensive.
HMOs and EPOs tend to have lower monthly premiums. Since the in-network providers all agree on the pricing level for their services, this helps the HMO/EPO to keep costs low.
These plans also tend to have lower copays and coinsurance than other health insurance plans. However, it’s important to remember that these lower costs are gained by using in-network providers.
Related Article: 3 Questions To Ask Before Picking Your Company's Health Insurance
In part due to their out-of-network benefits, POS plans typically come with slightly higher premiums. PPOs, which give members the most choice in terms of which providers they see, often have still higher monthly premiums and copays. They also almost always have an annual deductible, or an amount the insured member must pay out-of-pocket before the insurance plan kicks in and pays any claims. HMOs, EPOs, and POS plans often have no deductible or a low deductible.
That said, PPO members can save money by seeing doctors that are within the PPO network, as out-of-network providers will generally cost more.
Primary Care Physicians (PCP) and Referrals
As mentioned before, one key difference between these different healthcare plans is whether they require members to choose a primary care physician (PCP) to manage their overall care.
HMOs require members to choose a PCP to manage their overall care. The PCP must be in the HMO’s network, and this doctor will be the provider you see any time you need medical treatment.
If you need to see a specialist, you would first visit your PCP, who would then refer you to an in-network specialist. Or, to put it another way, you may not be covered for a visit to a specialist without that referral from the PCP. Still, the HMO provides an affordable option and can be good for people who don’t mind using a PCP to manage their care.
POS plans also typically require members to choose a PCP. Some POS plans require referrals from this PCP to see specialists, but others are “open access,” meaning that patients do not need referrals.
Both EPOs and PPOs do not require members to choose a PCP, and they don’t require referrals to see specialists. PPO members can see any doctor or provider they like, in- or out-of-network.
The flexibility of POS and PPO is nice for people who already have a doctor they like, since they won’t have to switch to one in-network. It’s also helpful for people who travel and want coverage, because members can see doctors outside of their local network as needed.
Related Article: Should Small Businesses Offer Dental and Vision Insurance?
The Bottom Line: Pick What Fits Your Team
Remember that every health insurance plan varies. It’s important to carefully review each one as it pertains to your teams’ needs.
If you and your employees desire plans that prioritize lower cost, HMO or EPO insurance may be a good fit, particularly if people just want basic medical care.
If your employees prefer more choices for care and don’t mind paying more for it, a PPO tends to offer greater flexibility. POS plans can offer the best of both worlds, with access to a national network of providers at rates more competitive with HMO or EPO plans.
If you’re looking for affordable health insurance for your team, Justworks can help. Take a look at our benefits and explore the plans we offer access to.
Learn more with Justworks’ Resources
Scale your business and build your team — no matter which way it grows. Access the tools, perks, and resources to help you stay compliant and grow in all 50 states.